
The New Way To Manage
Prior Authorizations
UltraTouch® Verify
Organize, submit, analyze, and improve prior authorizations, all in one place with the support of real people.
Don't settle for submission alone.
What if prior authorization technology could do more than just decrease approval times?
Most health systems and pharmacies struggle to manage their prior authorizations. Plenty of resources exist that help submit PA's or get them approved quicker, but few can reduce the workload, prevent organizations from hiring, offer insights into payer behavior, or help answer hard questions when confusion inevitably arises.
The Complete Prior Authorization Solution
Designed, developed, and supported by D2's team of healthcare leaders, UltraTouch® Verify is a workflow-focused platform and a complete prior authorization solution. From built-in smart protocols, to monitoring your team's efficiency, to analyzing payer behavior, UltraTouch Verify offers unmatched insight and control over your organization's prior authorization processes.
Revolutionary PA Intelligence
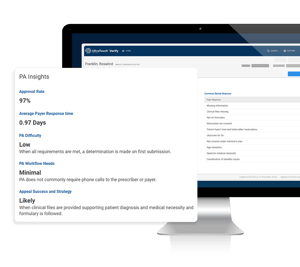
UltraTouch Verify's newest feature, PA Insights™, is the industry's first prior authorization support tool offering in-line workflow and protocol insights as you initiate and process PAs. Supported by the digital analysis of tens of thousands of PAs, their determinations, and their process workflows, PA Insights offers integrated intelligence including:
- Approval rate
- PA difficulty & workflow needs
- Common denial reasons
- Appeal success & strategies
- Average payer response time
- Custom enhancements based on industry and partner needs

Your Team of Prior Authorization Certified Specialists™
UltraTouch® Verify is supported by a team of 100% Prior Authorization Certified Specialists™ that serve as an extension of your own. We ensure you never tackle a difficult PA alone and are ready at any hour to:
- Speak with payers on your behalf
- Notify you of lingering prior authorizations
- Consult with you about ways to improve processes and efficiency
- Improve your experience on the Verify platform

Reimagine your prior authorization processes.
VerifyPA
VerifyPA™ is a feature of UltraTouch Verify that streamlines prior authorizations that need input from the prescriber. This secure, HIPAA-compliant portal simplifies the process by enabling electronic communication of information needed to satisfy a prior authorization.
VerifyPA reduces time-to-therapy for patients while improving workflow efficiency within the UltraTouch Verify platform.
Patient Eligibility & Product Coverage
UltraTouch Verify's eBV provides a tiered Eligibility API that delivers the precise data depth you need, ranging from essential routing keys to enriched payer intelligence. This flexible technology is matched with adaptable service levels, allowing you to choose between standard operational support or a strategic concierge partnership to align with your business goals.

Grow Your Business with UltraTouch Verify
- Organize
- Collaborate
- Process
- Submit
- Analyze
- Improve
Every Detail, All In One Place
UltraTouch Verify hosts a single, organized dashboard with every prior authorization. It’s easy to see where in the process each PA is, understand the history of patient care, minimize reauthorization time, and eliminate double work.
Collaboration Without Confusion
UltraTouch® Verify makes it easy to work together on a PA regardless of staff turnover, PTO or various roles and responsibilities. Work history is documented and time is automatically tracked for each PA along the way, helping to identify process inefficiencies and opportunities for improvement or training.
Smart Protocols Focused On First-Time Submission Approval
UltraTouch® Verify hosts smart protocols that are continually refined to provide the best path for single submission approval, and can be customized upon request. If trends are noticed by our e-services team, form protocols and alerts are developed.
Optimized For Your Workflow, Tracked By Our Team
Prior authorizations can be submitted into Verify manually or through automated processes (ex. EHR integration, APIs, etc.) Once submitted, all prior authorizations are tracked by the E-Serivces team to ensure quick movement from payers.
Growth-Enabling Reporting Tools
UltraTouch® Verify has detailed, customizable reporting capabilities that give our partners insight into their internal processes, payer behavior, therapy requirement trends, etc. In addition, UltraTouch® Verify and the E-Services team can work directly with you to develop custom reports that will help your business.
More Than Just a Prior Authorization Platform
UltraTouch® Verify serves our partners as not just technology, but a trellis to grow their organization on. With our Prior Authorization Certified Specialists by your side, Verify's protocols and workflows are refined and improved over time, allowing patient care to once again be the focus of your time.

The UltraTouch® Suite
Face accreditation head-on with D2's patient management technology - a single platform that collects, organizes, and catalogs patient data optimized for compliance standards.
Explore Patient ManagementReimagine patient engagement with automated and customizable patient outreach - getting more patients on therapy, getting them on therapy quicker, and keeping patients on therapy longer.
Explore EngageD2 Insights
Never stop learning about how the industry is shifting; explore our insights and grow alongside us.

